The Golden Years Guide to Understanding Your Blood Pressure
Why Blood Pressure Readings for Seniors Deserve Your Full Attention
Blood pressure readings for seniors are a critical health marker — and understanding yours could be one of the most important things you do this year.
Here’s what you need to know at a glance:
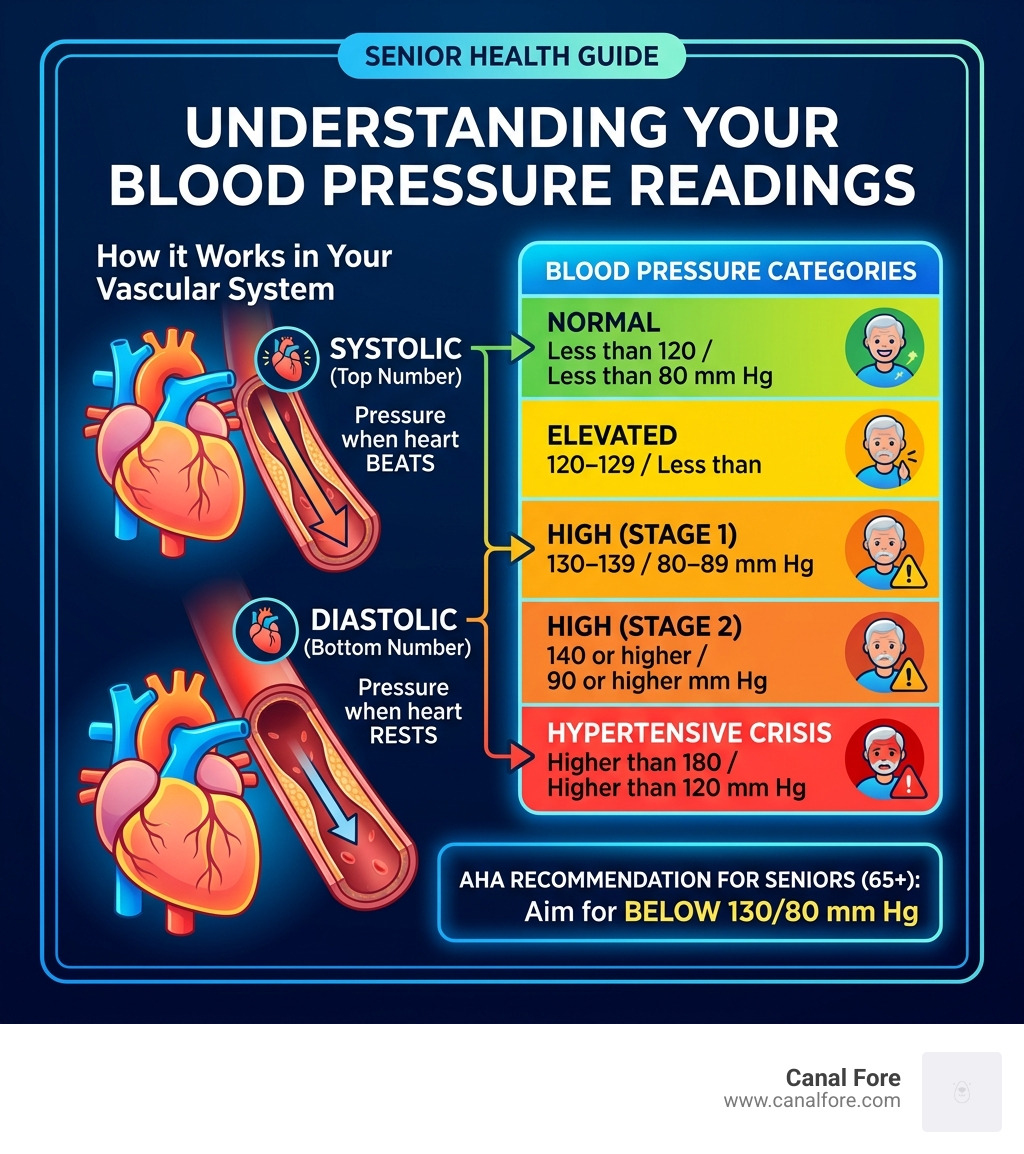
| Blood Pressure Category | Systolic (mm Hg) | Diastolic (mm Hg) |
|---|---|---|
| Normal | Less than 120 | Less than 80 |
| Elevated | 120–129 | Less than 80 |
| High (Stage 1) | 130–139 | 80–89 |
| High (Stage 2) | 140 or higher | 90 or higher |
| Hypertensive Crisis | Higher than 180 | Higher than 120 |
The American Heart Association recommends that adults aged 65 and older aim for a blood pressure reading below 130/80 mm Hg.
Between 70% and 80% of older Americans have high blood pressure. Yet most of them feel completely fine. That’s why doctors call it “the silent killer” — it causes serious damage to your heart, brain, and kidneys long before any symptoms show up.
Blood pressure is measured in two numbers:
- Systolic — the top number, measuring pressure when your heart beats
- Diastolic — the bottom number, measuring pressure when your heart rests between beats
Both numbers matter. But for adults over 50, the systolic number is especially important — because aging arteries tend to stiffen, which drives that top number up.
This guide breaks down exactly what healthy blood pressure looks like for older adults, why it changes with age, and what you can do to protect yourself.
What Are Normal Blood Pressure Readings for Seniors?
As we navigate our 60s, 70s, and beyond, our bodies change, and so do the benchmarks for our health. When we talk about blood pressure readings for seniors, we are looking at the force of blood against the walls of the arteries. This is measured in millimeters of mercury, abbreviated as mm Hg. This unit comes from the old-school manual gauges that used actual mercury to measure pressure. While we use digital monitors today, the terminology remains.
According to the American Heart Association (AHA) and the American College of Cardiology, the “gold standard” for most adults over 65 is a reading of less than 130/80 mm Hg. However, we must understand that “normal” is a range, not a single static number.
If your reading is consistently 115/76, you are in a great spot. If it starts creeping into the 120-129 range (systolic), you’ve entered the “Elevated” category. This is a wake-up call to look at lifestyle habits before you hit Stage 1 Hypertension (130-139/80-89). To get a better sense of where you stand, you can view this Elderly Blood Pressure Chart: What’s Considered Normal by Age? to see how these numbers are categorized.
Understanding Normal blood pressure readings for seniors
For many years, it was thought that “100 plus your age” was an acceptable systolic blood pressure. In 2026, we know better. Extensive research has shown that keeping blood pressure lower is significantly more beneficial for the heart and brain.
The AHA guidelines for those 65 and older are quite clear: aim for under 130/80 mm Hg. This applies to most seniors who are living independently and are relatively healthy. We’ve seen that What the New Blood Pressure Guidelines Mean for Older Adults often sparks a conversation about how “intensive” treatment should be.
While the average 60-year-old male might see a reading of 133/69 and a female might see 139/68, these are averages, not necessarily “ideals.” The goal is to keep the pressure low enough to prevent damage to the delicate vessels in the brain and kidneys, but high enough to ensure you don’t feel dizzy when you stand up.
Special Considerations for the Frail Elderly and Those Over 80
While 130/80 is the general target, we must practice what geriatricians call “individualized care.” For our seniors over 80, or those who are considered frail, the rules of the game change slightly.
If we push blood pressure too low in a frail person, we risk orthostatic hypotension. This is a sudden drop in blood pressure when someone stands up, which can lead to dizziness and dangerous falls. In these cases, a doctor might set a more relaxed target, perhaps 140/90 or even 150/90 mm Hg.
Geriatricians often look at the “whole person.” If a senior is already taking eight different medications, adding two more just to shave five points off their systolic reading might do more harm than good due to side effects. We always prioritize quality of life and safety—especially fall prevention—when determining the right blood pressure target for someone in their late 80s or 90s.
Why Blood Pressure Changes as We Age
It’s a fact of life: as we get older, our blood vessels change. Think of your arteries like a garden hose. When the hose is new, it’s flexible and expands easily when the water is turned on. Over time, that hose might get stiff or “hardened.”
In our bodies, this is called artery stiffening. As the large arteries lose their elasticity, they can’t buffer the pulse of blood coming from the heart as well as they used to. This increases vascular resistance, which naturally pushes the systolic blood pressure higher. Additionally, years of plaque buildup (atherosclerosis) can narrow the “pipes,” requiring more pressure to move blood through the system. You can learn more about these biological shifts from the High Blood Pressure and Older Adults | National Institute on Aging.
Isolated Systolic Hypertension in Older Adults
This is the most common form of high blood pressure in seniors. Isolated Systolic Hypertension (ISH) occurs when your systolic (top) number is high (130 or above), but your diastolic (bottom) number is normal or even low (below 80).
Why does this happen? It’s almost entirely due to that loss of artery elasticity we mentioned. Because the arteries are stiff, the pressure spikes when the heart contracts (systolic). But because the vessels don’t “snap back” efficiently, the pressure drops significantly when the heart rests (diastolic).
ISH is a major risk factor for strokes and heart disease. It can also cause symptoms like dizziness or lightheadedness, particularly if the diastolic pressure drops too low, depriving the brain of oxygen-rich blood for a split second.
Gender Differences in Senior Hypertension
Gender plays a fascinating role in how hypertension develops. Before age 55, men are more likely to have high blood pressure. However, after menopause, the risk for women increases sharply.
By the time we reach age 75, the statistics are eye-opening:
- 81% of women over 75 have hypertension.
- 73% of men over 75 have hypertension.
The loss of estrogen, which helps keep blood vessels flexible, is thought to be a major reason why women “catch up” and eventually surpass men in hypertension rates. For a deeper dive into these trends, check out the Blood Pressure Chart Per Age & Gender | Baptist Health.
Health Risks and the Importance of Intensive Control
High blood pressure isn’t just a number on a screen; it’s a direct threat to our longevity. When blood pressure readings for seniors remain high, the constant “pounding” on the vessel walls leads to:
- Stroke: High pressure can cause a vessel in the brain to burst or become blocked.
- Heart Disease: The heart has to work harder to pump against the pressure, leading to an enlarged heart or heart failure.
- Vascular Dementia: Tiny “micro-strokes” caused by high pressure can damage brain tissue over time.
- Kidney Damage: The kidneys rely on healthy blood vessels to filter waste; hypertension is a leading cause of kidney failure.
For more information on why managing these numbers is so critical, read What’s the best blood pressure target for older adults?.
The SPRINT Trial and Brain Health
One of the most important pieces of medical research in recent years is the SPRINT trial (Systolic Blood Pressure Intervention Trial). This study looked at over 9,000 adults aged 50 and older.
The findings were revolutionary. The study showed that lowering systolic blood pressure to a target of 120 mm Hg (intensive control) compared to a target of 140 mm Hg (standard control) significantly reduced the risk of cardiovascular events and death.
Perhaps even more exciting for seniors is the link to brain health. The SPRINT-MIND sub-study found that intensive blood pressure control significantly reduced the risk of developing mild cognitive impairment, a precursor to Alzheimer’s disease. In short: protecting your heart is one of the best ways to protect your mind.
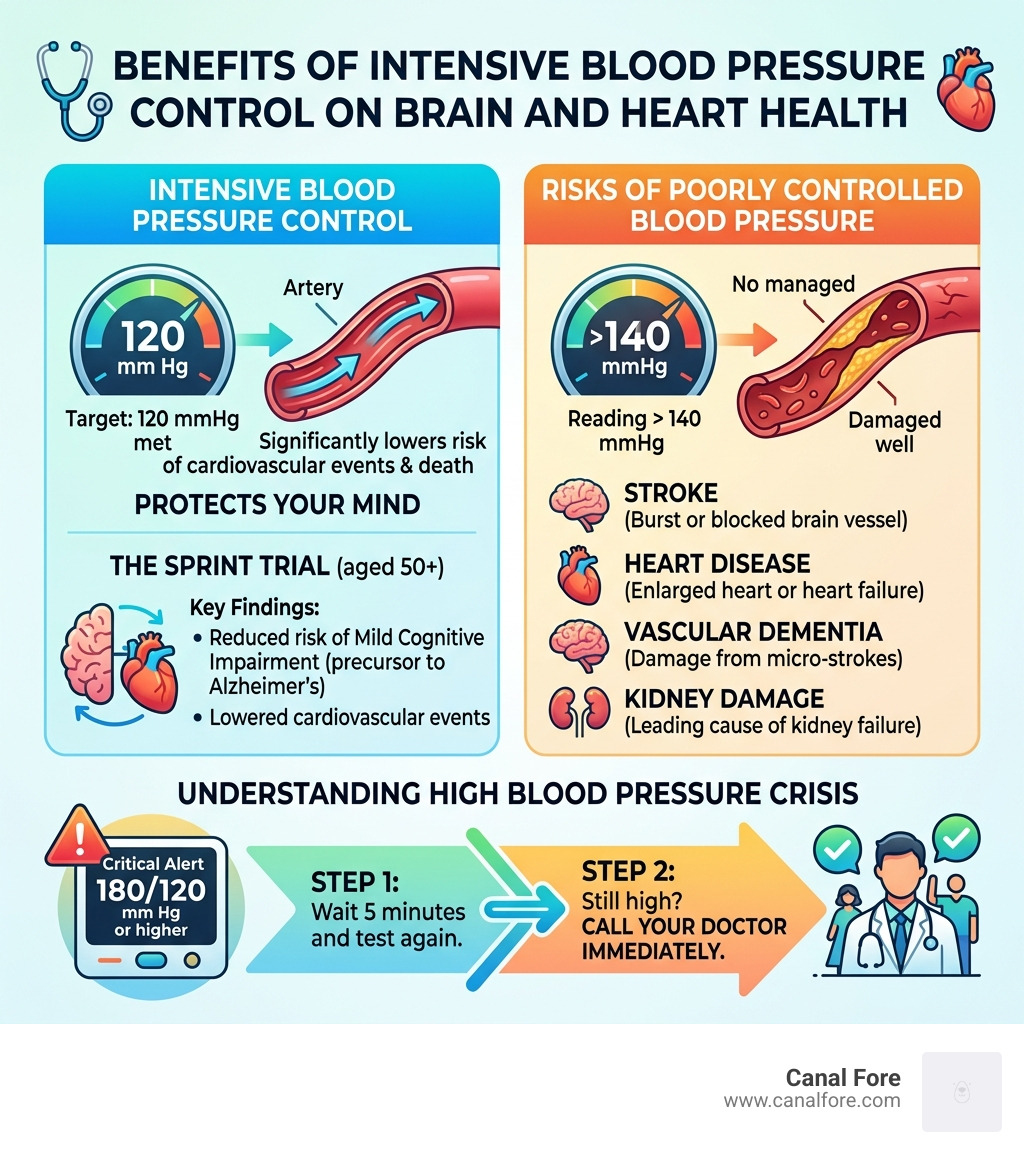
When blood pressure readings for seniors Indicate a Crisis
Sometimes, blood pressure doesn’t just creep up; it skyrockets. This is known as a Hypertensive Crisis.
If your home monitor shows a reading of 180/120 mm Hg or higher, we recommend waiting five minutes and testing again. If the second reading is still that high, it’s time to call your doctor.
If you have a reading of 180/120 and you are experiencing any of the following, call 911 immediately:
- Severe chest pain
- Shortness of breath
- Sudden change in vision
- Difficulty speaking or numbness/weakness
- Severe headache
This is a medical emergency that requires immediate intervention to prevent a stroke or organ damage.
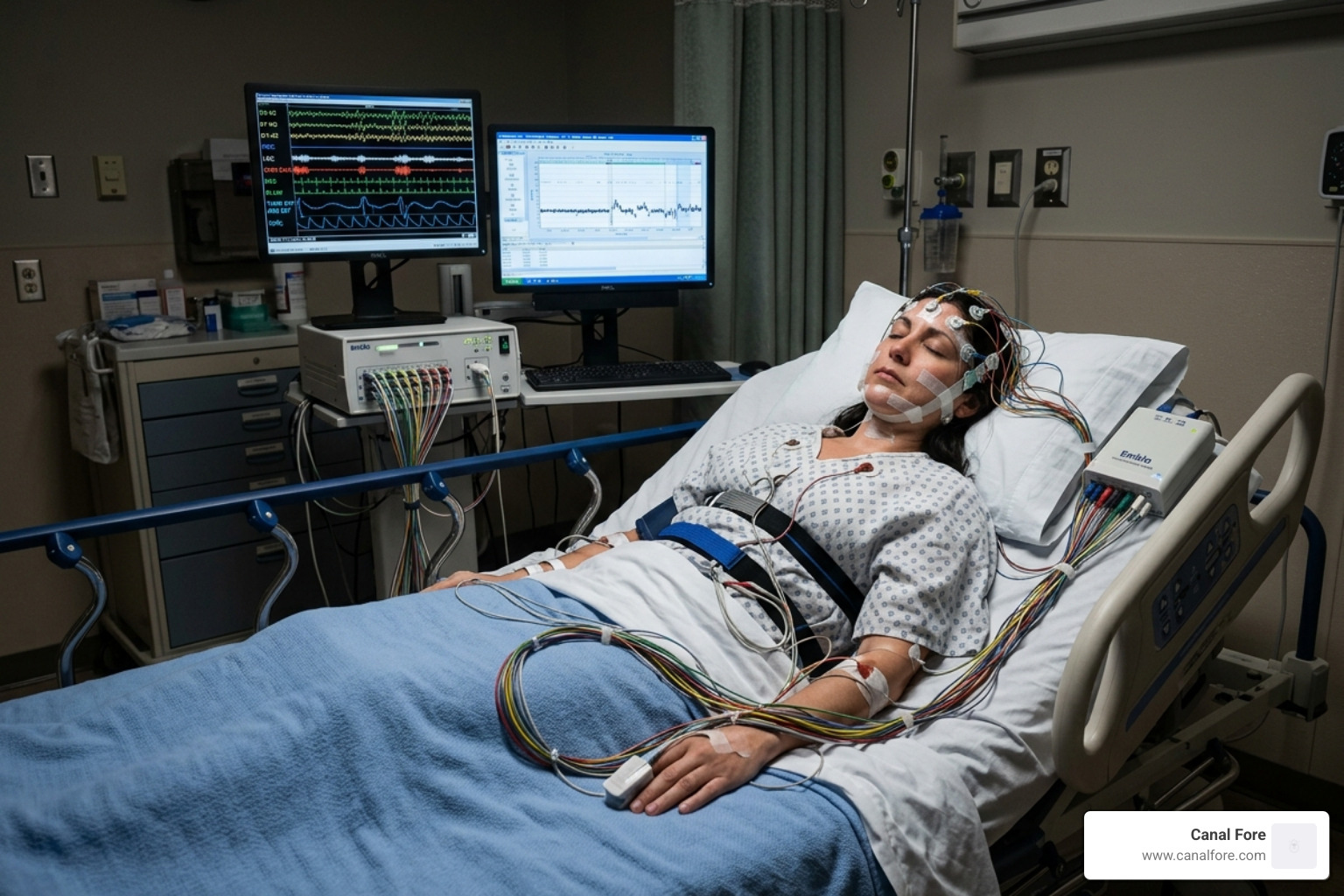
How to Get Accurate blood pressure readings for seniors at Home
Relying solely on the blood pressure check at the doctor’s office can be misleading. Many seniors experience “White Coat Hypertension,” where the stress of being in a medical setting causes their pressure to spike.
This is why we strongly encourage home monitoring. To get it right, you need the right equipment. Upper arm monitors are generally much more accurate than wrist or finger monitors for seniors. We suggest looking for a monitor that has been “validated” for accuracy.

Best Practices for Home Monitoring
To get the most accurate blood pressure readings for seniors, follow these steps every time:
- Prepare: Don’t smoke, drink caffeine, or exercise for 30 minutes before the test.
- Empty your bladder: A full bladder can actually add 10-15 points to your reading!
- Sit correctly: Sit in a chair with your back supported and your feet flat on the floor (don’t cross your legs).
- Support your arm: Your arm should be resting on a flat surface (like a table) at heart level.
- Rest: Sit quietly for 5 minutes before pressing the “start” button. No talking!
- Double up: Take two or three readings about one minute apart and average them.
The Role of Caregivers in Monitoring
If you are caring for an aging loved one, you are an essential part of their health team. We recommend keeping a simple log (either on paper or in an app) of their blood pressure readings.
Notice the trends. Is the pressure always higher in the morning? Does it drop significantly after they take their medication? Sharing this trend analysis with their doctor is much more valuable than a single reading.
Caregivers can also help ensure medication adherence. It’s easy for a senior to forget a pill, but for blood pressure management, consistency is everything. If the senior is experiencing dizziness or falls, check their blood pressure while they are sitting and again after they have been standing for two minutes. This can help identify orthostatic hypotension.
Managing Hypertension Through Lifestyle and Medication
The good news is that high blood pressure is one of the most treatable conditions we face. It often starts with lifestyle changes.
- The DASH Diet: (Dietary Approaches to Stop Hypertension) emphasizes fruits, vegetables, whole grains, and lean protein. It is low in salt and saturated fat.
- Salt Sensitivity: As we age, our bodies become more sensitive to salt. Even small reductions in sodium can lead to big drops in blood pressure.
- Physical Activity: We recommend at least 150 minutes of moderate exercise per week. This could be as simple as a brisk 30-minute walk five days a week.
- Potassium Intake: Foods rich in potassium (like bananas, spinach, and sweet potatoes) help the body flush out sodium and ease tension in your blood vessel walls.
- Stress Management: Chronic stress keeps your heart in “overdrive.” Meditation, deep breathing, or even spending time with a pet can help.
Common Medications for Senior Hypertension
If lifestyle changes aren’t enough, we turn to medication. Most seniors require two or more types of medication to reach their target. Common types include:
- Diuretics: Often called “water pills,” these help the kidneys remove excess salt and water.
- ACE Inhibitors: These help relax blood vessels by blocking the formation of a natural chemical that narrows them.
- Calcium Channel Blockers: These prevent calcium from entering the heart and blood vessel cells, allowing vessels to relax.
- Beta Blockers: These reduce the workload on the heart and open up blood vessels.
We always monitor for side effects like fatigue, cough, or swollen ankles, as these can affect a senior’s willingness to stay on their treatment plan.
Long-term Support in Senior Living
At Canal Fore, we understand that managing blood pressure can feel like a full-time job. That’s why our communities are designed to take the weight off your shoulders.
We offer professional monitoring, ensuring that blood pressure readings for seniors are taken accurately and regularly. Our culinary teams focus on heart-healthy, low-sodium meals that actually taste good, and our wellness programs make getting those 150 minutes of exercise a fun, social experience. Having a team of experts to watch for trends and manage medications can provide incredible peace of mind for both the senior and their family.
Frequently Asked Questions about blood pressure readings for seniors
What is a normal reading for a 70-year-old?
For a healthy 70-year-old, the target is generally at or below 120/80 mm Hg, with the threshold for hypertension starting at 130/80. However, your doctor may adjust this based on your specific health history.
Can drinking more water lower my blood pressure?
Actually, drinking plenty of water is usually recommended to help with low blood pressure or to prevent dehydration-related spikes. While staying hydrated is essential for overall health, it isn’t a direct “cure” for hypertension. However, replacing sugary sodas with water can help with weight loss, which does lower blood pressure.
Is 140/90 considered high for someone over 80?
In the general population, yes. However, for a very elderly or frail person, a doctor might decide that 140/90 is an acceptable “compromise” to avoid the side effects of aggressive medication, such as fainting or falling. Always follow your physician’s specific guidance.
Conclusion
As we move through 2026, the science is clearer than ever: keeping a close eye on your blood pressure is a cornerstone of healthy aging. While it’s natural for our vessels to stiffen over time, we have more tools than ever to manage this change.
By understanding your blood pressure readings for seniors, staying active, eating well, and working closely with your healthcare team, you can significantly reduce your risk of stroke, heart disease, and dementia.
If you or a loved one are finding it difficult to manage these health needs at home, we are here to help. Our communities provide the structure, nutrition, and professional support needed to keep those numbers in the healthy zone. Find a senior living community today and let us help you make your golden years your healthiest years.